Viral comments (22): Zika and animals: We do not know much!
The Zika virus is an emerging virus (ZIKV), because right now it rides on Aedes genus mosquitoes colonizing new geographic areas, but it’s been around us openly over 60 years (it is noted on a recent study that the three variants that circulate nowadays, two African and one from Asia, have a common origin back in 1920, but we cannot go beyond that time) and probably hundreds or thousands of years in their natural hosts … which we have not yet fully identified.
The first description of Zika came from a rhesus monkey, a sentinel animal hanging from a tree in a cage, in a program on Yellow Fever research of the Rockefeller Foundation in the Zika forest in Uganda. On the 18th of April, 1947, this monkey showed fever symptoms and days later was taken to the central laboratory in Entebbe, Uganda capital. Its serum was extracted and inoculated into mice intracranially. At day 10 all mice were sick. From the brains of those mice a transmissible filterable agent which we now call Zika virus, was isolated. A note, remember that viruses, in the beggining of its discovery, were called filterable agents to distinguish them from infectious bacterial agent which were retained by filters; viruses were as liquid, that percolated through the filter and could continue transmitting infection in the obtained filtrate.The following year, 1948, Zika was also isolated in Zika forests from Aedes mosquitoes, Aedes africanus. A few years later, in 1956, also it was shown that the Zika virus could be transmitted by Aedes aegypti, which was experimentally inoculated and was able to transmit the virus to mice and a monkey, in laboratory conditions.
Then, researchers saw an eclipse phase in the mosquito: they let mosquitoes fed on infected blood with a heavy viral load, around 108, ie 100.000.000 Zika viruses per ml. On day 0, day of the intake, each individual mosquito contained about 105,5 virus, which would mean about 300,000 virus. But at the 5th and 10th day, the virus could not be isolated from mosquitoes; from days 15 and 20, they returned to contain the virus at initial concentrations, close to 105.0 maintaining this level of infectivity up to day 60, more than 6 weeks later. The extrinsic incubation period of the virus in the mosquito, therefore would be between 10 and 15 days. However, this experiment demonstrated the possibility of laboratory transmission but not ecological transmission since we lack real and consistent data on the levels of viremia in animals (human and non-human primates); if those viremia levels were low then perhaps those experiments were wrong from the beginning in its approach.
Initial serological tests in human population in the vicinity of the virus isolation location, Central Africa, detected neutralizing antibodies to Zika in a 6% (6 of 99 individuals) thereof. An approximately identical proportion to that found in monkeys (1 positive out of 15 analyzed). Between 1951 and 1981, serological evidence of Zika infection in human populations was described in Uganda, Tanzania, Sierra Leone, Central African Republic, Gabon, Egypt, and jumping continent in India, Malaysia, Thailand, Philippines and Indonesia and Vietnam. The prevalence of neutralizing antibodies was quite variable. Thus, in Nigeria, where Zika was isolated from human population studies in 1968 and between 1971-1975, 40% of people had neutralizing antibodies against the virus. Indeed, also a 50% had antibodies against yellow fever and 46% against West Nile Virus, which could reflect a more intense circulation of the latter two viruses in the population. Differentially in Lombok, Indonesia, further serological study indicated that 9 of 71 (13%) human volunteers had ZIKV neutralizing antibodies, which may reflect a more recent circulation … or a less intense one. In this same study sera from horses, cattle, goats, ducks, chickens, wild birds, bats and rats in the same location was tested for antibodies against viruses such as Japanese encephalitis virus, Chikungunya, Ross River and Zika viruses. Regarding Zika, positivity was not detected.
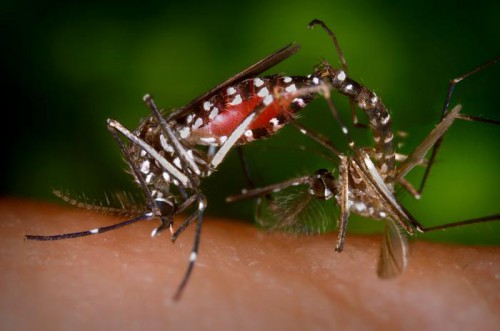
At the mosquito level, ZIKV has been isolated from Ae. africanus, Ae. apicoargenteus, Ae. luteocephalus, Ae. Aegypti, Ae vitattus. and Ae. Hensilii, the predominant mosquito species present in Yap Island during the outbreak of the Zika disease at 2007. However, with regard to the latter, no epidemiological link was proven since researchers could not detect ZIKV in any mosquito on the island during the outbreak.
It seems evident that primates (including human beings) are susceptible to infection, and thus may show clinical symptoms and generate antibodies. In tests that followed its detection/isolation it was found that other species such as rats, guinea pigs and rabbits showed no clinical signs of infection after intracranial inoculation with Zika virus in laboratory conditions. However this is not the normal way in for ZIKV entry, it rather would require an infected mosquito bite elsewhere than in the brain. And the occurrence of neutralizing antibodies was not studied. It must be recalled that for 80% of infected individuals the infection courses sub-clinically, with no apparent symptoms. In subsequent studies antibodies against Zika have indeed been detected in rodents; therefore these animals suffer infection and can produce antibodies.
We are faced with a patchwork of experiments that almost raises more questions than answers. Now we know that Zika is spread through mosquito bites and it seems clear that nonhuman primates act as vectors… but we cannot exclude other mammals. I am sure that mosquitoes do not make many distinctions and certainly viruses don’t, provided they can find a suitable environment and adequate cellular receptors. In fact, with high likelihodd, we have an enzootic cycle, maintaining the virus in populations of nonhuman primates and rodents and perhaps other yet undetermined guests in the original forests… which has resulted in a spillover into human population. And now, the least we can say is that Zika has come into scene to stay.
But this, this is another story.













